|
Work with your provider to reach your optimal levels You should talk to a thyroid doctor about how to best time your testing both in frequency and time of day. It is not uncommon for the dosage of levothyroxine to be changed multiple times throughout the pregnancy to keep up with the stress the pregnancy puts on the body.Īsk all the questions you want through our chat appīeyond long term changes in your body, there is evidence that thyroid hormone levels naturally fluctuate and follow diurnal rhythm. The TSH should continue to be checked every six weeks throughout the pregnancy. In order to avoid ever experiencing symptoms of hypothyroidism during pregnancy, a patient should have her TSH checked before becoming pregnant if possible, and again six weeks after conception. However, in the hypothyroid patient, the thyroid likely will not be able to increase production and even with levothyroxine supplementation, TSH levels may rise out of the patient’s optimal range. In a healthy individual, the thyroid can keep up by producing more hormone. Women need about 45% more thyroid hormone during pregnancy to maintain their optimal TSH level. One of the most common causes of change in thyroid hormones is stress, and one of the most common prolonged causes of stress on the body during a woman’s life is pregnancy. Your optimal thyroid level changes as your body and lifestyle do. Based on the reference ranges given above for the “normal” reference range, the following gives the optimal range that most thyroid patients report feeling their best at: TSH 0.5-2.5 uIU/mL, free T3 3.8-4.4 pg/mL, free T4 1.4-1.77 ng/dL, anti-TPO 0.0 IU/mL, and anti-TG 0.0 IU/mL.Īgain, these values are not an end-all-be-all and not everyone’s optimal level will fall between these ranges, but this gives you an idea of the discrepancy between the calculations that the labs make based on their overall patient population when making a reference range and how patients with hypothyroidism are feeling clinically.ĭoes my optimal level change at different times of life? You and your provider should strive to reach this optimal level, adjusting your medication appropriately until you are at a level that makes you feel your normal self again. Since the optimal thyroid function level is the level at which you feel your best at, it varies for each person. The approximate reference range for antithyroglobulin antibodies is 0-0.9 IU/mL. 
This makes them of limited value in patients with Hashimoto’s thyroiditis, but it is still important to make note of their role. Antithyroglobulin antibodies are not specific to one disease of the thyroid and are even found in 1 in 10 normal individuals. Thyroglobulin is a protein produced by the cells of the thyroid that also assists in the production of thyroid hormones. The second antibody that attacks the thyroid and can lead to an autoimmune disease is antithyroglobulin antibody. The reference range for anti-thyroid peroxidase antibodies is 0-34 IU/mL. Anti-thyroid peroxidase antibodies attack TPO resulting in decreased TPO activity and decreased production of thyroid hormones. Thyroid peroxidase (TPO) is an enzyme present mainly in the thyroid that is turned on by TSH and helps with the production of T3 and T4. There are a couple of antibodies that, if present, can cause suspicion for an autoimmune disease of the thyroid as there should be no antibodies attacking our own cells. When you get your results from your at-home thyroid test kit, you will see your TSH, free T3, free T4, and TPO antibody levels.įor thyroid stimulating hormone (TSH), which is the hormone that signals synthesis and release of T3 and T4 from the thyroid gland, the normal range is approximately 0.45-4.50 uIU/mL.įree T3 and Free T4, which are the hormones produced and released by the thyroid gland, have ranges of 2.0-4.4 pg/mL and 0.82-1.77 ng/dL, respectively. 
The Endocrine Society recommends that TSH levels be maintained between 0.2- 4.5 mU/L) are associated with increased risk for miscarriage and should be avoided in early pregnancy.Oops! Something went wrong while submitting the form.Īs discussed above, “normal” levels for thyroid blood tests can differ among labs, but there are general ranges that only vary slightly from lab-to-lab. Thyroid hormone requirements increase with pregnancy and many women with pre-existing hypothyroidism need an increase in their thyroid hormone doses in the first trimester of pregnancy. Inadequately treated hypothyroidism has been associated with negative pregnancy outcomes. Miscarriage: this occurs when a baby dies in the first few months of a pregnancy, usually before 22 weeks of pregnancy. 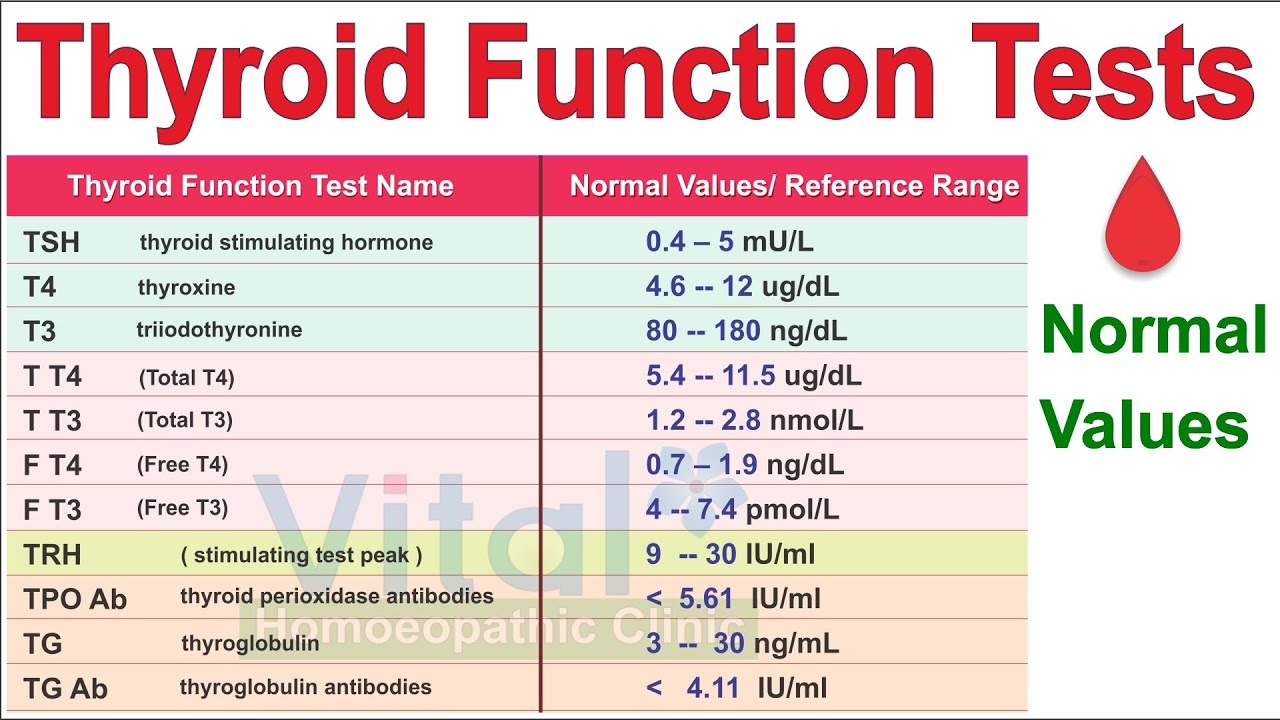
TSH: thyroid stimulating hormone – produced by the pituitary gland that regulates thyroid function also the best screening test to determine if the thyroid is functioning normally.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
